Introduction
Cervical Facet Joint Syndrome(CFJS) is a common condition that often goes underdiagnosed, yet it plays a critical role in the management of chronic neck pain.
The cervical facet joints, also known as zygapophyseal joints, are essential for stabilizing and facilitating movement in the cervical spine. Pain from these joints can arise due to traumatic injuries, such as whiplash, or degenerative changes like osteoarthritis.
CFJS is a significant contributor to axial neck pain. This highlights the importance of this issue for healthcare providers.
A comprehensive approach to diagnosis is crucial, as it involves a combination of clinical evaluation, imaging studies, and diagnostic medial branch blocks, since no single test can provide a definitive diagnosis. Management strategies can encompass conservative therapies such as physical therapy and medication, as well as more advanced procedures like radio frequency neurotomy.
This article provides an evidence-based overview of CFJS, exploring its anatomy, prevalence, Aetiology, pathophysiology, clinical presentation, diagnostic methods, and treatment approaches.
It aims to equip healthcare professionals with the knowledge necessary to accurately diagnose and effectively manage this condition, ultimately improving patient outcomes.
Relevent Clinical Anatomy
See Cervical Anatomy & Facet Joints for a comprehensive coverage of the Anatomy.
Prevalence
Cervical facet joint syndrome is a significant contributor to chronic cervical spine pain, with studies reporting a prevalence of approximately 55% (95% CI: 49%–61%) among patients with chronic, non-specific cervical spine pain referred for interventional pain management.[1] However, the false-positive rate for a single diagnostic block ranges from 27% to 63%.[2] Macroscopic examination of the cartilage surface of the facet joints suggests that the prevalence of facet joint degeneration is likely high and tends to increase in severity with age.[3]
Aetiology
Cervical Facet Joint Syndrome (CFJS) arises from a combination of mechanical, inflammatory, and degenerative factors that impact the cervical facet joints.[4]
By comprehending these factors, we can better address and manage this condition.
The primary aetiological contributors:
1) Traumatic Injuries
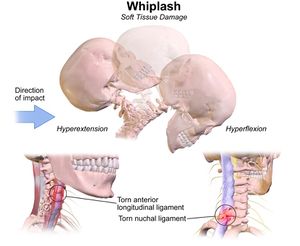
- Whiplash Injuries: Sudden movements, such as hyperextension or hyperflexion of the neck during motor vehicle accidents, are common causes of CFJS.
These whiplash-associated disorders (WAD) can lead to excessive compression of the facet joints or strain on the capsular ligaments, resulting in pain.
- Fractures or Dislocations: Acute cervical trauma from sports injuries or falls can lead to facet fractures, joint dislocations, or tears in the capsular ligaments.
- Capsular Ligament Strain: Overuse or sudden trauma to the capsular ligaments can lead to inflammation and pain.
2) Degenerative Changes
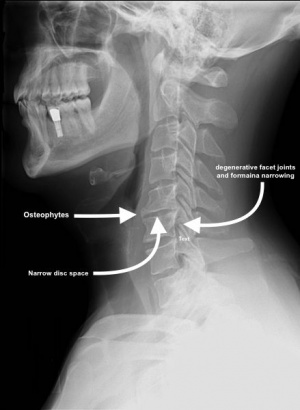
- Osteoarthritis: As we age, the degeneration of articular cartilage and subchondral bone can lead to joint space narrowing, osteophyte formation, and increased stress on the facet joints.
- Disc Degeneration: The "three-joint complex theory"[5] suggests that degeneration of intervertebral discs leads to reduced disc height, altering load distribution and increasing wear on the facet joints.
3) Inflammatory Processes
In response to joint injury or degeneration, inflammatory mediators like substance P and calcitonin gene-related peptide (CGRP) are released, sensitizing pain receptors within the facet joint capsule.
4) Postural or Biomechanical Stress
Chronic poor posture often due to prolonged screen time or repetitive neck movements, can place undue stress on the facet joints, leading to micro trauma.
5) Other Contributing Factors
- Age: The degenerative changes in facet joints typically begin after our second decade of life and progress with age.
- Previous Cervical Surgery: Adjacent segment disease following spinal fusion can increase stress on nearby facet joints.
- Obesity: Excess weight can place additional mechanical load on the cervical spine, increasing the likelihood of joint degeneration.
Pathophysiology
The pathophysiology encompasses both structural and neurochemical processes, as detailed below:[6]
1) Joint Anatomy and Biomechanics
- Facet Joint Structure: The cervical facet joints are diarthrodial synovial joints formed by the articulation of the superior articular process of one vertebra and the inferior articular process of the adjacent vertebra. Each joint is encapsulated by a fibrous capsule, lined with a synovial membrane, and includes articular cartilage and meniscoid structures.
- Normal Biomechanics: These joints permit controlled movement of the cervical spine, enabling flexion, extension, lateral bending, and rotation. They are responsible for bearing axial loads and play a critical role in maintaining spinal stability.
- Pathological Changes in Facet Joints : Traumatic or repetitive stress, in conjunction with degenerative changes, can disrupt normal joint biomechanics, leading to abnormal loading conditions, capsular strain, and potential joint instability.
2) Pain Mechanisms
- Mechanical Irritation: Excessive compression or strain on the capsular ligament, arising from trauma (for example, whiplash) or degenerative alterations, may activate nociceptors within the joint capsule, resulting in pain.
- Synovial Meniscoids: Inflammation or pinching of the synovial folds (meniscoids) within the joint can also contribute to pain.
- Inflammatory Mediators: Injured facet joints release various inflammatory substances, including:
- Substance P and Calcitonin Gene-Related Peptide (CGRP): These neuropeptides enhance nociceptor sensitivity and amplify pain signaling.
- Cytokines: Localized inflammation can exacerbate tissue damage and perpetuate the pain response.
3) Neural Innervation and Pain Referral
- Innervation of the Facet Joints: Each cervical facet joint is innervated by the medial branches of the dorsal rami of the spinal nerves located above and below the joint. For instance, the C5-C6 joint is innervated by the medial branches of the C5 and C6 dorsal rami.
- Referred Pain Patterns: Pain originating from cervical facet joints is frequently referred to specific regions based on the affected joint segment:
- C2-C3 Joint: This joint may refer pain to the occipital region and upper cervical spine.
- C5-C6 Joint: Referred pain from this joint is often experienced in the lower cervical spine, shoulder, or scapular region.
4) Degenerative Changes
- Cartilage Breakdown: Degeneration of articular cartilage may result in joint space narrowing, increased friction, and osteophyte formation.
- Capsular Thickening: Chronic inflammatory processes can lead to fibrosis and thickening of the joint capsule, which reduces joint mobility.
- Altered Biomechanics: A reduction in intervertebral disc height can increase axial loading on the facet joints, further accentuating degenerative changes.
5) Whiplash-Associated Pathology
During a whiplash injury, the lower cervical spine may undergo hyperextension while the upper cervical spine flexes, resulting in an "S-shape" motion.
This atypical movement causes:
- Compression of the inferior articular process of the superior vertebra against the superior articular process of the inferior vertebra.
- Strain on the capsular ligament due to excessive extension, followed by a recoil effect upon returning to a neutral position, which may cause micro tears.
6) Chronic Pain Mechanisms
The Chronic Pain Mechanisms in cervical facet joint Syndrome (CFJS) results from :
- Central Sensitization: Prolonged activation of nociceptors in the facet joints can lead to increased sensitivity within the central nervous system, resulting in persistent pain despite the healing of the initial injury.
- Muscle Spasm and Dysfunction: Reflex muscle guarding surrounding the cervical spine further limits mobility and perpetuates the cycle of pain.
Physical Examination And Diagnosis
Cervical Facet Joint Syndrome (CFJS) is a clinical diagnosis that requires careful evaluation due to its nonspecific symptoms and overlap with other cervical spine disorders.
A complete Cervical Spine Assessment is a must for an accurate diagnosis of CFJS.
A combination of history-taking, physical examination, imaging studies, and diagnostic injections is essential for an accurate diagnosis.
1. Clinical History
- Pain Characteristics: Patients typically describe dull, aching axial neck pain, which may radiate to the shoulders, upper back, or occipital region. Pain often worsens with:
- Cervical extension or rotation.
- Prolonged static postures (e.g., sitting or driving).
- Sudden neck movements.
- Trauma History: A history of whiplash injury or hyperextension trauma is common.
- Activity-Related Pain: Activities requiring repetitive neck movements or prolonged screen use may exacerbate symptoms.
2. Physical Examination
While no single physical examination test definitively diagnoses CFJS, several findings can support the clinical suspicion:
- Palpation:
- Localized tenderness over the cervical facet joints.
- Muscle tightness in the paraspinal or trapezius regions.
- Range of Motion (ROM):
- Pain during cervical extension and rotation, especially when combined.
- Limited ROM due to discomfort.
- Manual Pressure Tests:
- Pain reproduction with manual compression or posterior-anterior pressure over the suspected facet joints.
- Neurological Exam:
- CFJD is typically free of neurological deficits, helping differentiate it from cervical radiculopathy or myelopathy.
3. Diagnostic Imaging
Imaging studies are not specific for CFJS but can rule out other conditions and provide supportive evidence:
- X-rays:Radiographs in the neutral, flexed, and extended positions, should be obtained and the degree of movement measured in patients suspected with cervical facet syndrome. Horizontal movement of one vertebral body on the next should not exceed 3.5 mm, and the angular displacement of one body on the next should be less than 11°. These criteria may not always be applicable in the younger athlete, in whom ligamentous laxity may accentuate these measurements. More specifically, the normal translation of the OA joint in the sagittal plane is insignificant.
- Useful for detecting osteoarthritis, fractures, or instability.
- Flexion-extension views can reveal dynamic instability in trauma cases.
- Computed Tomography (CT):
- Offers detailed visualization of bony structures and facet joint osteophytes.
- Magnetic Resonance Imaging (MRI):
- Identifies soft tissue abnormalities, including capsular thickening and synovial inflammation.
- Helpful in excluding discogenic or neural compression pathology.
4. Diagnostic Injections
Diagnostic blocks are the gold standard for confirming CFJS:
- Medial Branch Blocks:
- Intra-Articular Injections:
- Local anesthetic is injected directly into the facet joint under fluoroscopic guidance.
- Provides additional confirmation when medial branch blocks are inconclusive.[7]
- Double-Block Technique:
To improve diagnostic accuracy, two injections with different anesthetics (e.g., lidocaine and bupivacaine) are performed on separate occasions. Pain relief consistent with the duration of each anesthetic supports the diagnosis.[7]
Differential Diagnosis
CFJD symptoms overlap with other cervical spine conditions. A thorough evaluation should rule out:
- Cervical Disc Herniation.
- Cervical Radiculopathy or Myelopathy.
- Cervical strain or sprain.
- Spinal Stenosis.
- Myofascial Pain syndrome.
- Occipital Neuralgia.


تعليقات
إرسال تعليق